This cold weather has induced a Winter brain freeze. I've been working on a post about old school trauma blankets, but trouble with writer's block has slowed me down-if you could even call my foolishness writing!
I have zero insight about which of my posts are popular with readers. Sometimes my idea of a good post only comes up with a hundred views or less. Subjects that seem on the lame end of the spectrum end up with a thousand or more views. "Go figure," as I've heard youngsters exclaim when something doesn't make sense.
Drum roll...please. My most viewed post of 2017 was this gem with about 2,200 views.
http://oldfoolrn.blogspot.com/2017/01/not-on-my-back-table.html (Caution contains disturbing image.) I did not have the appropriate insight and judgment when publishing this little gem to add the disturbing content disclaimer and this got me blacklisted on some referral sites. My bad (another expression I learned from you clever youngsters,) and a thousand pardons for my crude behavior. I will try to contain my inherent barbarity in the future.
Wishing you the best New Year yet!
"The amazing thing about young fools is how many survive to become old fools" ..... Doug Lauer
Friday, December 29, 2017
Thursday, December 21, 2017
Technology-The Perils of Early Adoption
 |
When knowledge, experience and technology
fall into place concurrently amazing things happen.
Sometimes this takes time. |
The latest and greatest in new technology provides contemporary
ample fodder for advertisements and bragging rights. Lack of experience and knowledge with technological capabilities can produce some unforeseen problems; antibiotics cure infections, but microorganisms fight back, X-ray treatments of enlarged thymus glands in children gave rise to cancer later in life, and bone marrow transplants for metastatic breast cancer were a big disappointment.
This is my personal tale of an encounter with a brain MRI done back in the good old days of the 1980's when these gigantic imaging machines were called NMRI-the "N" was short for nuclear. The neuro radiologists of today were likely in Kindergarten and ordinary run-of-the-mill radiologists interpreted these vintage scans.
After a fusillade of neuro problems including confusion, right upper extremity weakness, and visual field distortions I had one of those new fangled NMRI imaging studies performed. While I was reclined in the tight confines of that sewer pipe of a machine, I was aware of a commotion commencing in the procedure room. Turns out mine was one of the very first NMRIs that showed significant pathology at this facility and an audience had gathered to witness the premier event. I walked into the NMRI room and left on a Gurney for an acute neuro ward-not a good sign. Here is the radiologist's interpretation.
The striking finding is an increase in T2 signal intensity in the right occipital area and to a somewhat lesser extent in the right frontal area. Differential might include CNS lymphoma, primary demyelinating process, encephlopathic or infectious etiology less likely. Correlation with clinical findings is suggested.
Now the real fun began. Neurosurgery was consulted and felt the scan was consistent with a glioma and a stereotactic biopsy would be necessary to determine the type. Alas, this was impossible because of the unavailability of a non-ferrous stereotactic head frame. Using the standard head frame would wind up with my head plastered to the magnet like a bug on a windshield. I remember thinking about calling Jack Kevorkian to see if he could squeeze me in as the prognosis seemed more grim as time passed, but there were many more consultants waiting in the wings so let's wait and see.
Next on the parade of consultants was a neurologist whose primary area of expertise was MS, of course he concluded that MS was the diagnosis and a spinal fluid study for monoclonal antibodies would be the confirmation. The studies later proved negative for monoclonal antibodies so the diagnosis was changed from MS to "demyelination syndrome," whatever that means.
Let's consult a clinical pharmacologist to get his opinion. I was taking Azulfidine for Crohns Disease and a review of the literature suggested an encephlopathic process could be a result of taking this drug. The final diagnosis: Azulfidine induced encephalopathy. Stopping the Azulfidine made no difference in my neuro status, but jump started the Crohns, not a pleasant situation.
I slowly recovered and started backing away from follow-up appointments, figuring that whatever it was would take its course. My neurosurgeon died about 5 years ago and I started to marvel at my survival skills having outlived him. He had given me a prognosis of 5-7 years.
So 28 years after the original excitement a
A genuine neuro radiologist interpreted this MRI and there was none of that old school beating around the bush. This lady knew what she was looking at, no bones about it. I certainly could have benefited from her expertise 28 years ago. Here is her impression.
abnormal foci of T2 hyperintensity within the subcortical and periventricular white matter are much greater in size and number in the right cerebral hemisphere compared to the left. There is a more confluent area of abnormal T2 hyperintensity posterior to the right lateral ventricle. The asymmetrical appearance of these lesions effectively rules out classic multiple sclerosis. This MRI is indicative of an acute disseminated encephalomyelitis.
It's nice to have a definitive diagnosis even though it required a 28 year wait. Some problems cure themselves if you can wait them out. Time is the most valuable commodity and the neuro Gods have cut me a break. I'm still vertical and my foolishness remains intact but sometimes I wonder about my cognitive abilities.
Thursday, December 14, 2017
Nursing Awards - Emmitt Knows Where They Belong
 |
Proud winners of a nursing award. At least
their trophy has relevance-looks like a bath basin.
|
It's too bad that some nurses lack Emmitt's judgment and discretion regarding meaningless, phoney baloney awards worth their weight in wormwood. Hospitals of today often have a shrine-like area where garish gold plaques are displayed honoring a select group of nurses. Nothing wrong with this concept if it gives recognition to deserving nurses who have honed their technical skills to help patients, but frequently the awarding entity is far removed from patient care and has little insight into bedside nursing excellence or comforting patients. Physicians, administrative nurses (if you could even call them nurses,) insurance companies, and the nurse academic/ office sitter complex all have very minimal working knowledge of what makes a good bedside nurse. Doctors just love nurses who know their rightful place and never question orders or call them up in the middle of the night. Administrative types view nursing through the distorted lens of corporate goals and please don't get me started on office sitters of any permutation. Discretion is the better part of valor, I keep muttering to myself. Sometimes it's better to keep my foolish mouth shut.
We certainly had nothing like this when I was a nurse. Our instructors and mentors (if you could call them that) always stressed that the satisfaction of helping patients recover from injury or ailment had to come from within. If a trauma patient walked out the door or a patient's pain was relieved, you did a good job and that was your reward. In their mind nursing was a calling and required self motivation which was also a good reason for paying nurses a poverty wage. If you are looking for good time Charley back slapping rewards or big money you are in the wrong profession.
As a public service the OFRN institute for nursing practice is going to separate the wheat from the chaff when it comes to awards for nurses. If you notice any of the following words or combination of words in the criteria or award title, its of dubious distinction: influential, pinnacle, showcase, emerging, distinguished, rising star, engagement, transformational, breakthrough, paradigm, cameo, illustrious, or eminent. It's time to go above and beyond or even eschew these nonsensical awards. It's time to take a lesson from Emmitt Smith and deposit these chucklehead awards in their rightful place.
Here are a few worthy nursing awards that have straightforward criteria and reflect nursing as it's clinically practiced, untainted from pie-in-the-sky bafflegab.
The Last Nurse Standing Award... An endurance award of sorts to the scrub nurse that can hang in there on one of those knee aching surgeries that start before sunrise and end after sunset and I'm talking about Chicago - not the Arctic circle. My personal best is close to 8 hours on a complex trauma and that's not even worth mentioning because my mentor Nancy went for close to 12 hours on a Whipple with complications. She deserves a standing ovation and a well deserved trip to the bathroom.
The Stink Finger Statue... Goes to the nurse who never shied away from any mess-you name the body excretion and this nurse gets down to business, sans gloves. I really admired this nurse because almost everyone has an Achilles heal when it comes to messes, mine was that gooey blood/bone chip slurry mess left on the floor of the ortho room after a long, messy case. Blood..no problem, bone chips..no problem, but mix them together and the resultant ooze-like combo brought me to my knees every time. Thanks to Colleen and Gail for bailing me out on this one. You deserve this and remember to refrain from sniffing those fingers.
Venous Access King or Queen...goes to the best IV starter. Bring me your hypovolemic, phlebotic and sclerotic patient and I'll slide that angio cath in faster than you can say central line.
The Sailor Award...goes to the most fluent user of off color language. I usually avoided this one because it resulted in much childhood unpleasantness if caught uttering swearwords, but I some how felt a sense of relief when others spouted out colorful descriptive language. Nurse Felix deserves this award for coming up with the u;timate inclusive cuss word (sh++t,f**k.G++d**n it) all in one breath. What more can I say?
Most Likely to Cry...I always admired nurses that could do this. It's better than alcohol or drugs at diffusing sadness. The most I could come up with were a couple of stray tears, but at least I tried.
Most Kind nurse...We all know one of these. This nurse is nice to everyone and always sports an infectious smile that's even visible under a mask. As nurses age this trait seems to decline although I have met a couple of these angels in white who were well into their 60s. Rita you deserve this award if you can stop puffing on that Winston long enough to claim it.
The Walking Wounded...These tough nosed, hardened nurses can work through bone on bone hip joints, unremitting Crohns Disease, or even while on chemo for aggressive cancers. Tough as nails; the primary objective is to die at the bedside with their Clinic Shoes on. I did manage to scrub on a case one day after having impacted wisdom teeth removed and I was never so grateful that it did not involve oral surgery. The pain sharpened my senses, but I would not never, ever want anyone to work for this award.
A really good nurse will do whatever it takes to help a patient in need not because it's about award procurement, but because it's the right thing to do. The fact that the obsessive pursuit of awards leaves profound deficits in other areas of direct nursing care is a definite reality. Emmitt got it right.
As a public service the OFRN institute for nursing practice is going to separate the wheat from the chaff when it comes to awards for nurses. If you notice any of the following words or combination of words in the criteria or award title, its of dubious distinction: influential, pinnacle, showcase, emerging, distinguished, rising star, engagement, transformational, breakthrough, paradigm, cameo, illustrious, or eminent. It's time to go above and beyond or even eschew these nonsensical awards. It's time to take a lesson from Emmitt Smith and deposit these chucklehead awards in their rightful place.
Here are a few worthy nursing awards that have straightforward criteria and reflect nursing as it's clinically practiced, untainted from pie-in-the-sky bafflegab.
The Last Nurse Standing Award... An endurance award of sorts to the scrub nurse that can hang in there on one of those knee aching surgeries that start before sunrise and end after sunset and I'm talking about Chicago - not the Arctic circle. My personal best is close to 8 hours on a complex trauma and that's not even worth mentioning because my mentor Nancy went for close to 12 hours on a Whipple with complications. She deserves a standing ovation and a well deserved trip to the bathroom.
The Stink Finger Statue... Goes to the nurse who never shied away from any mess-you name the body excretion and this nurse gets down to business, sans gloves. I really admired this nurse because almost everyone has an Achilles heal when it comes to messes, mine was that gooey blood/bone chip slurry mess left on the floor of the ortho room after a long, messy case. Blood..no problem, bone chips..no problem, but mix them together and the resultant ooze-like combo brought me to my knees every time. Thanks to Colleen and Gail for bailing me out on this one. You deserve this and remember to refrain from sniffing those fingers.
Venous Access King or Queen...goes to the best IV starter. Bring me your hypovolemic, phlebotic and sclerotic patient and I'll slide that angio cath in faster than you can say central line.
The Sailor Award...goes to the most fluent user of off color language. I usually avoided this one because it resulted in much childhood unpleasantness if caught uttering swearwords, but I some how felt a sense of relief when others spouted out colorful descriptive language. Nurse Felix deserves this award for coming up with the u;timate inclusive cuss word (sh++t,f**k.G++d**n it) all in one breath. What more can I say?
Most Likely to Cry...I always admired nurses that could do this. It's better than alcohol or drugs at diffusing sadness. The most I could come up with were a couple of stray tears, but at least I tried.
Most Kind nurse...We all know one of these. This nurse is nice to everyone and always sports an infectious smile that's even visible under a mask. As nurses age this trait seems to decline although I have met a couple of these angels in white who were well into their 60s. Rita you deserve this award if you can stop puffing on that Winston long enough to claim it.
The Walking Wounded...These tough nosed, hardened nurses can work through bone on bone hip joints, unremitting Crohns Disease, or even while on chemo for aggressive cancers. Tough as nails; the primary objective is to die at the bedside with their Clinic Shoes on. I did manage to scrub on a case one day after having impacted wisdom teeth removed and I was never so grateful that it did not involve oral surgery. The pain sharpened my senses, but I would not never, ever want anyone to work for this award.
A really good nurse will do whatever it takes to help a patient in need not because it's about award procurement, but because it's the right thing to do. The fact that the obsessive pursuit of awards leaves profound deficits in other areas of direct nursing care is a definite reality. Emmitt got it right.
Friday, December 8, 2017
Ahh-The Good Old days
I got sick and tired of viewing that image of the traumatized (and that's putting it nicely) young man in my previous post. Kind of a foolish post and I should probably refrain from reading old posts. My proof reading skills are lacking to the extent when I go back over my post to correct errors, I make it even worse. Paradoxical indeed!
I've had this picture floating around and could not come up with a post that equals what it illustrates. I catch myself staring at it and daydreaming of the old days before patients were customers and hospitals became health care centers. It's so much nicer than that previous traumatic illustration. What was I thinking?
I've had this picture floating around and could not come up with a post that equals what it illustrates. I catch myself staring at it and daydreaming of the old days before patients were customers and hospitals became health care centers. It's so much nicer than that previous traumatic illustration. What was I thinking?
Caps, Rotary dial telephone, paper charts, and nurse attentively viewing a cathode ray tube monitor. I think I just heard that distinctive air bubble gurgle from a vented glass IV bottle as it infuses.
Tuesday, December 5, 2017
Who You Gonna Call?
 |
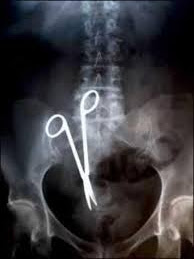
Dr. Slambows treatment plan would be to anesthetize and "succ" the above patient and then simply yank that nasty blade out. "Standby...if there is bleeding we will have to go in and find the bleeder, lets hope for the best." Dr. Slambow always called the standing around and waiting routine, "masterful inactivity."
I can't imagine the number of specialties that might be consulted today for a case like this. Here is the conversation between two residents considering the various consults that might be indicated.
"We better get an occuloplastic surgeon to see this tattooed knife target. That wound is pretty near the eye."
"No..I'm calling the ENT man, that toad sticker is obviously impacting his maxillary sinus. Maybe an oral surgeon too."
"What about that hospital directive advising a neurosurgery consult for any wound to the head?....That's not his head, that's his face I' calling the chief plastic surgery resident on call."
The straightforward approach would be a call to Dr. Slambow to quickly resolve the problem while the others are pontificating and checking the patients insurance coverage.
"
Thursday, November 30, 2017
Hospital Signage - Yesterday and Today
Visits to contemporary hospitals always throw me for a loop. The hodge-podge assemblage of signage is indeed mind boggling, at least for me. Practically every vertical surface or door has a sign of one sort or another dutifully posted. Guide signs, financial responsibility notices, warning signs, nursing award plaques (none of those back in my day, that's for sure,) and mystery signs that my foolish mind simply could not decipher.
I found myself asking myself, how in the world did old school hospitals function without the copious ( that "c" word is one of the all time favorite words of my generation of nurses) use of signs? The hospital building itself was without an identifying sign. It was completely unnecessary because everyone intuitively knew it was a hospital. A hospital was a hospital and everyone knew where it was. Does God sign the sky?
Walking through a modern hospital corridor with all those solid, opaque doors with confusing (at least to me) signage does cultivate a sense of mystery. When one of these modern, occlusive, door contraptions swing or magically whoosh open, I scramble to peak inside. I could have read the ever present, omniscient signage, but I like the feeling of being an explorer on an adventure. It's like a series of hidden little worlds where computers and electronic doo-dads seem to dominate.
Old hospitals were not like this. No signs necessary. You could sense where you were by the various olfactory, auditory, or visual cues. The radiology department was defined by the scent of photographic fixer and all those lead aprons hanging outside the mostly open doors. No mysteries here. Morgues and central supply were always in the basement and the ORs were always on the top. I rambled on about this in a previous post.
Emergency rooms were always on the same level as the street and there was a memorable sign nearby. Old school emergency triage began at street level and an actual sign began the process by a stern warning: AMBULANCE CASES ONLY. There was always an assemblage of police cars at the ER and I suspect hospital emergency rooms were one of the safest places in all of Chicago.
Hospital labs were easy to navigate. Everything was out in the open. Hematology was defined by the click-clck-click of manual tabulator gizmos used by the technicians to count the various lymphocytes and eosinophils in a sample. I used to love that sound because it reminded me of crickets. A bit of nature in the midst of an urban jungle. The microbiology department was easy to spot with banks of incubators and rows of microscopes. The chemistry lab division smelled, well chemical. You couldn't miss it. The hospital laundry was easy to find, just follow that lovely clean linen smell and as you got closer, little flecks of lint falling like snow clearly defined the locus.
Old hospitals had very few people just strolling through as outpatients because there were no outpatients. Any nurse would be all to happy to direct any lost soul moving about the halls so there was little need for signs. The loud, ubiquitous hospital paging system clearly announced visiting hours and instructions for hospital visitors. One of the greatest advances in modern hospitals is the absence of verbal loud speaker pages. They could really jangle your nerves.
Occasionally, a modern hospital sign will cause my foolish, old brain to crash in a state of persistent befuddlement. What the heck is an outpatient ICU?? I was completely bamboozled by a sign pointing the way to "Ambulatory Surgery." How in the world, I wondered, can you perform surgery on someone while they are walking around? I suspect it is a great way to prevent post op complications like atelectasis and clots, but do the benefits outweigh the risks of surgery in motion?
I' getting carried away here so I'll leave you with some contemporary hospital signage that got my attention and made my blood boil. The sign below serves to provide the patient with all the respect and dignity of a visit to Wal Mart. The remuneration request is for something that is an abstract concept concocted by an office sitting bean counter which contrasts with the mission of healthcare to provide tangible care for a person in need. Money and associated big business is what robbed both doctors and nurses of their status as caring professional care givers and relegated them to nothing more than dollar sign driven minions. It's a sin and a shame.
 |
| Signs were few and far between in vintage hospitals. |
I found myself asking myself, how in the world did old school hospitals function without the copious ( that "c" word is one of the all time favorite words of my generation of nurses) use of signs? The hospital building itself was without an identifying sign. It was completely unnecessary because everyone intuitively knew it was a hospital. A hospital was a hospital and everyone knew where it was. Does God sign the sky?
Walking through a modern hospital corridor with all those solid, opaque doors with confusing (at least to me) signage does cultivate a sense of mystery. When one of these modern, occlusive, door contraptions swing or magically whoosh open, I scramble to peak inside. I could have read the ever present, omniscient signage, but I like the feeling of being an explorer on an adventure. It's like a series of hidden little worlds where computers and electronic doo-dads seem to dominate.
Old hospitals were not like this. No signs necessary. You could sense where you were by the various olfactory, auditory, or visual cues. The radiology department was defined by the scent of photographic fixer and all those lead aprons hanging outside the mostly open doors. No mysteries here. Morgues and central supply were always in the basement and the ORs were always on the top. I rambled on about this in a previous post.
Emergency rooms were always on the same level as the street and there was a memorable sign nearby. Old school emergency triage began at street level and an actual sign began the process by a stern warning: AMBULANCE CASES ONLY. There was always an assemblage of police cars at the ER and I suspect hospital emergency rooms were one of the safest places in all of Chicago.
Hospital labs were easy to navigate. Everything was out in the open. Hematology was defined by the click-clck-click of manual tabulator gizmos used by the technicians to count the various lymphocytes and eosinophils in a sample. I used to love that sound because it reminded me of crickets. A bit of nature in the midst of an urban jungle. The microbiology department was easy to spot with banks of incubators and rows of microscopes. The chemistry lab division smelled, well chemical. You couldn't miss it. The hospital laundry was easy to find, just follow that lovely clean linen smell and as you got closer, little flecks of lint falling like snow clearly defined the locus.
Old hospitals had very few people just strolling through as outpatients because there were no outpatients. Any nurse would be all to happy to direct any lost soul moving about the halls so there was little need for signs. The loud, ubiquitous hospital paging system clearly announced visiting hours and instructions for hospital visitors. One of the greatest advances in modern hospitals is the absence of verbal loud speaker pages. They could really jangle your nerves.
Occasionally, a modern hospital sign will cause my foolish, old brain to crash in a state of persistent befuddlement. What the heck is an outpatient ICU?? I was completely bamboozled by a sign pointing the way to "Ambulatory Surgery." How in the world, I wondered, can you perform surgery on someone while they are walking around? I suspect it is a great way to prevent post op complications like atelectasis and clots, but do the benefits outweigh the risks of surgery in motion?
I' getting carried away here so I'll leave you with some contemporary hospital signage that got my attention and made my blood boil. The sign below serves to provide the patient with all the respect and dignity of a visit to Wal Mart. The remuneration request is for something that is an abstract concept concocted by an office sitting bean counter which contrasts with the mission of healthcare to provide tangible care for a person in need. Money and associated big business is what robbed both doctors and nurses of their status as caring professional care givers and relegated them to nothing more than dollar sign driven minions. It's a sin and a shame.
|
|
Thursday, November 23, 2017
Giving Thanks
| Thanks, Nancy |
I have lots to be grateful for and often think of those who helped me as a young nurse. Thanks to you Nancy Swabeck RN for your patience in sharing your skills as one of the most elite and skilled scrub nurses I have ever known. It sounds paradoxical, but as the pressure and anxiety came to a boil with unexpected problems your relaxed peacefulness and calm demeanor flourished. A life lesson to be sure.
Smooth and easy flowing movement of instruments with that last little burst of energy on approach to the surgeon's hand was her trademark, but it was anything but when I tried to replicate her ease of movement. Herkey, jerkey and uncertainty marked my initial efforts. "Keep at it. When you are gong through a surgical
Nancy was a cool headed natural problem solver when it came to instrument handling. I was always flummoxed by trauma cases that engaged two teams working simultaneously. My usual modus operandi involved setting up two separate Mayo stands and designating one as self service. Sometimes this worked when dealing with ortho, but always left one of the teams disgruntled with my lame efforts.
Nancy taught me how to mentally divide a single Mayo stand in two sections so as to serve double duty. Half for this service and the other half for that service. It worked but usually made my head spin. Later when we received brand new elevated neuro tables with just one huge work area, she taught me how to create an imaginary Mayo stand work area. I'm a slow learner so she went to the trouble of outlining a pretend Mayo stand with methylene blue. It worked like a charm. She always had an answer for everything.
The events of a long ago Thanksgiving are also on my mind when we had that brainstorm of a notion to cook a turkey in an autoclave. The tale of the autoclaved Thanksgiving turkey is on this blog somewhere and some day I will mater links.
I am also grateful to all of you who read my incessant foolishness. There are so many well written nursing blogs out there by bright, young, whippersnapperns that I hate to waste your time. At least I provide some cognitive diversity to the nursing world. Oops that sounds a bit grandiose so I better cease while I can. Thanks for your readership and a festive Thanksgiving to you and yours.
Sunday, November 19, 2017
Vintage Magnetic Therapy for Ocular Foreign Bodies
I just love gadgets and gizmos from the days of old school healthcare. Now this handy dandy device is something that I could have put to use this past summer. I'm a self-taught, self maiming, lumberjack of sorts and as I was happily sharpening one of my dull chains, a fragment of metal was hurled into my eyeball by the grinder. I dimwittedly thought my eyeglasses would provide ample protection, but that shiny shard found an indirect path to my eye. Metal shavings have tiny little barbs on them that can make removal difficult. I tried to irrigate that little devil, but it would not budge.
After a $600+ emergency room visit, the metal shaving was successfully removed. I tossed the antibiotic prescription into the circular file along with an opthamology consult and lived happily ever after.
Now if I had access to that device pictured above, the ER visit would have been unnecessary. When the American industrial age was in full swing it was commonplace for workers to experience problems with metal shavings impacting their eyes. An enterprising opthamologist devised the above piece of medical equipment. The foreign body victim positioned their eyeball over the cone shaped proboscis like business end of this machine and the doc activated the electromagnet. PRESTO.. the metal shaving was liberated from the eyeball. I don't even want to think about the end result if the metal shaving was retro-ocular. Would the entire eyeball be pulled out? Hmm..I guess discretion is the better part of valor when using devices like this.
I've been attempting to figure out if the illustration on the right is just for demonstration or is this the outcome of treating a platoon of steelworkers after a blast furnace mishap?
Tuesday, November 14, 2017
Nursing Diagnosis - An Aimless Pursuit
Your patient suddenly loses consciousness, blows his pupils with a narrowing pulse pressure and
has the beginnings of decerebrate posturing. What's your diagnosis nurse?
"This patient is experiencing hypovigilance secondary to disruption in the flow of energy resulting in a disharmony of the mind, body, and/or spirit." Say what nurse? Old time diploma students never dabbled in this high minded, academic activity of the modern nurse diagnosticians, quite the contrary, we were sternly advised, "Nurses do not diagnose." This resulted in many deferrals to "Ask your doctor."
We were well versed in acute clinical contingencies (Ha..Ha...I can talk just like you smarty pants nurse diagnosers) and knew exactly what to do if the patients under our care had problems.
Verigo on arising-back to bed...A hemorrhaging arm laceration-slap a blood cuff on while the resident scrambles for hemostats...Hypoglycemic..Have some orange juice...A sluggish chest tube-milk it. It's really just plain old common sense.
A bona fide diagnosis is based on objective and measurable data, not the whim of a nurse wordsmith spouting off gobbledegook. The evidence supporting the diagnosis would enable different practitioners to come to the same conclusion. I think that those folks a lot smarter than I call it inter- rater reliability.
Nursing diagnoses grant objective status to subjective information. When subjectivity is confused with fact and treatments based on unfounded assumptions are implemented, bad things can happen such as that infamous 1-10 pain scale.
When nursing transitioned from a diploma based hands oneducation training to an academic setting, office sitter, nurse big shots had to come up with entities to differentiate themselves. They came up with three humdingers that are indeed, unique to nursing. Nursing research, which, more accurately should be called clinical research if the purpose is to improve clinical care. We don't have doctor research. Nursing theory of which I have written jabbered about in a previous post and finally nursing diagnosis.
These discursive disciplines have one thing in common. They are unique to nursing and difficult for other healthcare entities to understand. If the end game is to be a valuable, contributing member of a collaborative, team effort they fall short. Lots of nurses, especially old fools like me cannot comprehend them so maybe we should drop the nursing from nursing diagnosis and work toward a common goal. Diagnosis that is based on objective fact and guides healthcare workers toward effective treatment.
Nursing is all about common sense and using what you know to directly and appropriately helping patients. Having a nursing life that involves only intellectual and down right incomprehensible material is not a good way to live. Some folks think that mastering complex linguistic feats and fancy talk is going to make them look smart and sophisticated. Truly smart nurses have a high sense of humility and plain talk that really does help patients overcome illness or mishaps. .
has the beginnings of decerebrate posturing. What's your diagnosis nurse?
"This patient is experiencing hypovigilance secondary to disruption in the flow of energy resulting in a disharmony of the mind, body, and/or spirit." Say what nurse? Old time diploma students never dabbled in this high minded, academic activity of the modern nurse diagnosticians, quite the contrary, we were sternly advised, "Nurses do not diagnose." This resulted in many deferrals to "Ask your doctor."
We were well versed in acute clinical contingencies (Ha..Ha...I can talk just like you smarty pants nurse diagnosers) and knew exactly what to do if the patients under our care had problems.
Verigo on arising-back to bed...A hemorrhaging arm laceration-slap a blood cuff on while the resident scrambles for hemostats...Hypoglycemic..Have some orange juice...A sluggish chest tube-milk it. It's really just plain old common sense.
A bona fide diagnosis is based on objective and measurable data, not the whim of a nurse wordsmith spouting off gobbledegook. The evidence supporting the diagnosis would enable different practitioners to come to the same conclusion. I think that those folks a lot smarter than I call it inter- rater reliability.
Nursing diagnoses grant objective status to subjective information. When subjectivity is confused with fact and treatments based on unfounded assumptions are implemented, bad things can happen such as that infamous 1-10 pain scale.
When nursing transitioned from a diploma based hands on
These discursive disciplines have one thing in common. They are unique to nursing and difficult for other healthcare entities to understand. If the end game is to be a valuable, contributing member of a collaborative, team effort they fall short. Lots of nurses, especially old fools like me cannot comprehend them so maybe we should drop the nursing from nursing diagnosis and work toward a common goal. Diagnosis that is based on objective fact and guides healthcare workers toward effective treatment.
Nursing is all about common sense and using what you know to directly and appropriately helping patients. Having a nursing life that involves only intellectual and down right incomprehensible material is not a good way to live. Some folks think that mastering complex linguistic feats and fancy talk is going to make them look smart and sophisticated. Truly smart nurses have a high sense of humility and plain talk that really does help patients overcome illness or mishaps. .
Thursday, November 9, 2017
Poetic Artistry at it's Finest
Pretty please check out Underside of Nursing Blog (It's on my blogroll.) A poem dedicated to all the OldfoolRNs of the nursing world.
Thursday, November 2, 2017
Downey VA Introduces the Shoe Shine Nurse
Downey VA Hospital, the agencies largest psychiatric facility, had an aloof contingent of highly
educated, office-sitting nurses dedicated to grinding out an assortment of directives, memos, and program notes to lowly staff nurses for implementation.. These administrative hot shots even had their own building complete with plush Karastan carpeting, air conditioning and fancy pictures on the walls. A far cry from the dingy, smoke filled wards with cyclone fencing and bars on all the windows where staff nurses practiced. These office bound nurses never ventured far from their comfortable habitats, but their word became law out on the wards.
Examples of adjunctive therapy include: psychodrama where the patient acts out a scripted scenario under staff direction, token economy where the patient earns rewards and privliges as outlined by the staff, exercise group involving that old 1..2..bend and grunt routine, and work details such as the "spoon factory" where listless patients dutifully inserted plastic spoons in plastic bags for 8 hours at a stretch.
These adjunctive therapy all share a common thread and that's top/down delivery. A group leader instructed patients in a rigid, authoritarian manner.This did little to establish trust or facilitate communication.
Something different was needed here to demonstrate trust and caring. As I surveyed the ward, I noticed most of the patients were wearing scuffed and dull leather shoes. The ubiquitous athletic shoe was decades in the future. Low and behold, off in a distant corner, a little used and neglected shoe shine bench sat gathering dust.
Suddenly an epiphany popped into my head. The next day on the way to work, I stopped by the local Ben Franklin store (remember those?) and purchased a few tins of Florshiem paste shoe polish. After gathering a few worn out T-shirts, I was in the shoe shine business. That evening after the head nurse departed I initiated my shoe shine therapy program. I pulled that old relic of a shoe shine bench away from the wall, dusted it off and barked out, "OK fellas step right up. Let Nurse Fool shine your shoes. Let me buff them up to a brilliant shine in nothing flat."
Patients were reluctant at first, but after encouragement from the attendants, a few disheveled patients stepped forward and propped their lusterless shoes on the bench for an enthusiastic shine by my deft hands. At first I chatted with them about the condition of their shoes to get them talking. The role reversal and lateral delivery of care was off putting at first, but the shoe shine did help to build trust.
Caring and trust were in short supply at Downey VA, but at least I tried.
Thursday, October 26, 2017
One Flew Over the Cuckoo's Nest comes to Roost at Downey VA Hospital
 |
| Cuckoo's Nest Nurse Ratched on the silver screen at Downey VA |
One Flew Over the Cuckoo's Nest, based on a Ken Kesey novel, was a movie filmed on the back wards of an Oregon State Hospital for the Insane. It featured a down right despicable Nurse Ratched character that was domineering and abusive to her patients. She controlled everything on the ward from the TV to determining candidates for lobotomy. The scenes of the patients' on the ward was a spitting image of Building 66AB at Downey where I was working. Downey nurses, for the most part, were too burned out to dominate anyone. The modus operandi was just getting by until that Civil Service Retirement kicked in. There were no Nurse Ratcheds at Downey.
Downey had a rule that any closed ward group of patients must be accompanied by an RN on outings. I made it my personal mission to get these guys off that smoke filled, depressing ward as much as possible and organized walks, picnics, and even ball games. So when I heard about Cuckoos Nest being shown on movie night, I figured, what the heck? These guys are just about living the movie and I was curious how they would respond. I strolled onto the ward after supper and called out, "Movie night, who wants to go?"
Two dozen or so of the patients stepped up and we walked over to the theater. Sometime movies elicited shouting and bouts of unrestrained laughter, but during Cuckoo's Nest there was a strange silence from the crowd. The experience of sitting in a long term psychiatric hospital watching a movie filmed in such a location reminded me of watching a war movie in the middle of an active battlefield. Today one of the most overused words that pops up in contemporary banter is surreal.
Watching Cuckoo's nest at Downey VA with a group of schizophrenics was way beyond surreal. It was one of the most unusual experiences I've had as a nurse except perhaps for the time a patient filled his prosthetic leg with urine and asked for help putting it on. When I placed his stump in the prosthesis urine splashed everywhere to the delight of the young amputee.
After the movie ended, about half of the patients had no reaction what so ever, because the long term use of drugs like Thorazine had wiped out any trace of individual personality. A chemical lobotomy of sorts. Another group of patients had trouble separating reality from the movie characters and asked me to speak with Nurse Ratched to "straighten her out." The other small group identified with the characters and was delighted that someone had made a movie about them.
On the commute home, I kept thinking that I'm going to write about that Downey VA movie night experience down some day. I knew my lackluster writing skills would fail to communicate the bizarre nature of watching a movie imitating a mental hospital in a genuine metal hospital. At least I tried.
Thursday, October 19, 2017
Curved Surgical Instruments - What's the Deal?
One of the liberties of being "just a scrub nurse" was the privilege of asking dumb, foolish questions. When there was a lull in surgical action such as waiting for a phone call from pathology or passing time until an esoteric instrument was flashed, the time was ripe to pose philosophical queries to the attending surgeon. Surgeons could come up with some convoluted answers to foolish questions when they were caught off guard. Timing and delivery of the question was the key to obtaining an offbeat answer.
Here is a sampling of some questions I asked in a foolish attempt to resolve the greatest mysteries of the operating room; "Why do cloth shoe covers track blood on the floor a greater distance than new-fangled plastic disposable covers?... How normal is 0.9 saline?... Can you sleep on a mattress suture?... and perhaps the ultimate question... "Why is the working end of many surgical instruments curved?"
Here is a sampling of some questions I asked in a foolish attempt to resolve the greatest mysteries of the operating room; "Why do cloth shoe covers track blood on the floor a greater distance than new-fangled plastic disposable covers?... How normal is 0.9 saline?... Can you sleep on a mattress suture?... and perhaps the ultimate question... "Why is the working end of many surgical instruments curved?"
Friday, October 13, 2017
A Friday the 13th Foreign Body Mishap??
Tuesday, October 10, 2017
Thorazine - An Old Fashioned Cure-All
Thorazine was thought of as a revolutionary breakthrough medication similar to Penicillin when the FDA approved it's use in the early 1950's. It was the very first psychiatric medication useful in the treatment of schizophrenia. Before Thorazine, institutions used leather restraints, alternating cold and hot body packs and of course crude psychosurgery such as lobotomy.
In a bizzare side note Freud never received the Nobel prize for his work, but the fellow with that ice pick brain surgery got the call from Sweeden to come pick up his Nobel prize for lobotomy. Efforts to recall this Nobel have been unsuccessful.
Thorazine was discovered while searching for a cure for malaria and worked by blocking dopamine receptors in the brain - a chemical lobotomy. After Thorazine disables the dopamine receptors all sorts of bad things happen. Blocking dopamine does blunt the psychosis, but fooling around with neurotransmitters never has a happy ending. Akathesia (constant uncontrolled restlessness,) sustained muscle sasms leading to a debilitating constant muscle activity called tardive dyskinesia. I always thought of Thorazine as the equivalent of weeding a garden with a hand grenade. Sure the psychosis was blunted, but so was everything else that made the person an individual. These people were mere shells of human beings. The reeks and wrecks found on the backward of any long term psych hospital were not there only for their psychosis. The institutionalization and side effects of long term phenothiazine therapy were at fault too.
Thorazine was supplied in a wide range of dosage forms including; syrup, concentrate, injectable vials and even suppositories. On my first medication passing adventure at Downey VA I had a med card that indicated the patient was to receive 2000mg of Thorazine concentrate. I was taught the maximum dose was around 200 mg. How could a patient receive 2 grams of this potent tranquilizer and survive? I was told this was the correct dose and the patient acquired a tolerance over the decades and to go ahead and give it. The patient shuffled up to the med room, gulped it down and went about his business. Simply amazing.
Some of the long term Thorazine concentrate consumers requested the nasty tasting substance "straight." This meant giving the drug in a small medicine cup diluted with just a splash of tap water. The concentrate turned a brilliant shade of pink when the water was added and this was long before the color was associated with cancer survivors. Thorazine concentrate was just plain nasty smelling. Cracking that big brown tinted bottle unleashed a scent not unlike the Testors glue that I used as a youngster to assemble plastic model kits. We usually diluted it in a thick sugary substance called simply "citric." I doubted this tactic made it any more palatable, but at least it knocked some of the unpleasant smell down.
There is ample truth to the old adage that when there are 3 or more treatments for the same condition, none of them are effective. The pharmacologic corollary- If one drug is used to treat multiple divergent illnesses; it's not an effective drug. Here is an interesting hodge-podge of ailments that Thorazine was purported to cure in 1950s ads. A foolish panacea if I do say so.
Wow.. never realized Thorazine was such a miracle drug with an assortment of therapeutic applications. It did work well for nausea in small doses of 25mg, but patients never asked for a repeat dose. I always asked post-op patients if their nausea was relieved by the small dose of Thorazine and their reply was always something to the effect that it worked but made their mouth very dry and induced a profound malaise and general feeling of unwellness. "Don't give that to me again!" was a frequent request.
When drugs are touted as having so many uses I suspect it's because they don't work too well for anything. Of course this lesson has been well learned and would never happen today. HeHe.
In a bizzare side note Freud never received the Nobel prize for his work, but the fellow with that ice pick brain surgery got the call from Sweeden to come pick up his Nobel prize for lobotomy. Efforts to recall this Nobel have been unsuccessful.
Thorazine was discovered while searching for a cure for malaria and worked by blocking dopamine receptors in the brain - a chemical lobotomy. After Thorazine disables the dopamine receptors all sorts of bad things happen. Blocking dopamine does blunt the psychosis, but fooling around with neurotransmitters never has a happy ending. Akathesia (constant uncontrolled restlessness,) sustained muscle sasms leading to a debilitating constant muscle activity called tardive dyskinesia. I always thought of Thorazine as the equivalent of weeding a garden with a hand grenade. Sure the psychosis was blunted, but so was everything else that made the person an individual. These people were mere shells of human beings. The reeks and wrecks found on the backward of any long term psych hospital were not there only for their psychosis. The institutionalization and side effects of long term phenothiazine therapy were at fault too.
Thorazine was supplied in a wide range of dosage forms including; syrup, concentrate, injectable vials and even suppositories. On my first medication passing adventure at Downey VA I had a med card that indicated the patient was to receive 2000mg of Thorazine concentrate. I was taught the maximum dose was around 200 mg. How could a patient receive 2 grams of this potent tranquilizer and survive? I was told this was the correct dose and the patient acquired a tolerance over the decades and to go ahead and give it. The patient shuffled up to the med room, gulped it down and went about his business. Simply amazing.
Some of the long term Thorazine concentrate consumers requested the nasty tasting substance "straight." This meant giving the drug in a small medicine cup diluted with just a splash of tap water. The concentrate turned a brilliant shade of pink when the water was added and this was long before the color was associated with cancer survivors. Thorazine concentrate was just plain nasty smelling. Cracking that big brown tinted bottle unleashed a scent not unlike the Testors glue that I used as a youngster to assemble plastic model kits. We usually diluted it in a thick sugary substance called simply "citric." I doubted this tactic made it any more palatable, but at least it knocked some of the unpleasant smell down.
There is ample truth to the old adage that when there are 3 or more treatments for the same condition, none of them are effective. The pharmacologic corollary- If one drug is used to treat multiple divergent illnesses; it's not an effective drug. Here is an interesting hodge-podge of ailments that Thorazine was purported to cure in 1950s ads. A foolish panacea if I do say so.
 |
Hmm.. this might just work. Snow him on Thorazine and see if he makes it to the bar.
|
 |
| I wonder if her "serene detachment" persisted through the muscle spasms of tardive dyskinesia. |
 |
In my experience, Thorazine induced rapid, shallow respirations-not sure how well this would play out for asthmatics.
|
 |
Thorazine was known for it's hypotensive actions. Throw in an old time general
anesthetic with a Thorazine pre-op and watch the B/P drop like a lead balloon.
|
Wow.. never realized Thorazine was such a miracle drug with an assortment of therapeutic applications. It did work well for nausea in small doses of 25mg, but patients never asked for a repeat dose. I always asked post-op patients if their nausea was relieved by the small dose of Thorazine and their reply was always something to the effect that it worked but made their mouth very dry and induced a profound malaise and general feeling of unwellness. "Don't give that to me again!" was a frequent request.
When drugs are touted as having so many uses I suspect it's because they don't work too well for anything. Of course this lesson has been well learned and would never happen today. HeHe.
Wednesday, October 4, 2017
Las Vegas Massacre
Despite a rigidly enforced news blackout in my household, the really bad events have a way of surfacing. When I heard hundreds of people were victims of gunshot wounds in Las Vegas the logistics of treating this much trauma boggled my mind.
Three gunshot wounds were enough to wreak havoc in our busy Chicago OR. We used to mark preop X-rays with paper clips in a usually futile attempt to track trajectory. Projectiles can bounce or tumble after striking bone. The deflected path is difficult to assess. A box of paperclips lasted for years in the old time OR. I wonder if CT scans have eliminated the paper clip markers, but it's painful to think how many paper clips would be needed for hundreds of people.
The aftermath of mass shootings is becoming well scripted. The shooter is characterized as a psychotic madman which further unfairly stigmatizes the mentally ill. Politicians praise first responders and express sympathy for the victims. I heard one senator said it was to early in the investigation to consider legislative solutions. What more investigation is needed after learning the extent of the slaughter.
The gun rights folks will cite the second amendment which was crafted in an age of muzzle loaded weapons which took time to reload. I don't think our forefathers envisioned wide distribution of rapid fire assault type weapons, but gun folks might allude to the notion that it's a price that must be paid for freedom.
I wish folks could see how powerful guns are when bullets meet human flesh. Tiny entrance wounds give way to shredded small bowel and lacerated livers. If shooters knew how tired hands get loading hundreds of needle drivers or counting pack after pack of 4X4s they might see things differently.
I am so sorry for the victims and cannot fathom how surgeons and nurses could treat so much trauma.
Three gunshot wounds were enough to wreak havoc in our busy Chicago OR. We used to mark preop X-rays with paper clips in a usually futile attempt to track trajectory. Projectiles can bounce or tumble after striking bone. The deflected path is difficult to assess. A box of paperclips lasted for years in the old time OR. I wonder if CT scans have eliminated the paper clip markers, but it's painful to think how many paper clips would be needed for hundreds of people.
The aftermath of mass shootings is becoming well scripted. The shooter is characterized as a psychotic madman which further unfairly stigmatizes the mentally ill. Politicians praise first responders and express sympathy for the victims. I heard one senator said it was to early in the investigation to consider legislative solutions. What more investigation is needed after learning the extent of the slaughter.
The gun rights folks will cite the second amendment which was crafted in an age of muzzle loaded weapons which took time to reload. I don't think our forefathers envisioned wide distribution of rapid fire assault type weapons, but gun folks might allude to the notion that it's a price that must be paid for freedom.
I wish folks could see how powerful guns are when bullets meet human flesh. Tiny entrance wounds give way to shredded small bowel and lacerated livers. If shooters knew how tired hands get loading hundreds of needle drivers or counting pack after pack of 4X4s they might see things differently.
I am so sorry for the victims and cannot fathom how surgeons and nurses could treat so much trauma.
Tuesday, September 26, 2017
Surgical Instrument Identification Marking
 |
"Fetch me one of those thingamajigs
with the red and black marking tape"
|
It's not too hard to figure out the marking behavior of dogs, cats and bears, but to find the motivation for
I guess this is a convoluted way of saying you cannot tell what something is just by looking at it or using it. It's not all that difficult to learn the nomenclature of surgical instruments and have a general idea of how the instrument is used. A Penfield is a Penfield because that's what it is. The black and red tape is not what gives an instrument it's identity. So the instrument is the instrument, ineffable, a well defined entity completely independent of the strips of colored tape applied on the whim of an administrative wisenheimer. If you are working in the perioperative arena and don't know the identity of your instruments, the only steak you should be holding is a T-bone.
"We mark our instruments so as to organize them into sets for a specific case. Green/black markings mean the instrument is part of the fem-pop bypass tray," said nursing supervisor, Mary Marks-a-Lot
This is wrong headed thinking of the highest order. The surgery determines the type of instrument used not the instrument determining the surgery. The tail is wagging the dog with case specific instrument trays and the circulating nurse will be running like a whippet to the nearest autoclave to flash sterilize the instruments you really need for unexpected circumstances. I often fantasized about instrument marking misfits standing directly in front of the autoclave when I suddenly cracked the door after a flash sterilization cycle. Maybe a blast of scalding steam to their sensory regions would bring them to their senses.
Instruments used in case specific trays are also more subject to wear and tear because they are used in the same manner time after time. For maximum instrument life it's best to use them on a rotating basis with different cases through varying services. Auto mechanics don't have a breaker bar just for working on struts - they use it wherever it's needed. Surgical instruments should be used as needed and not assigned to a case specific use.
Scrub nurses have enough to keep track of; sponges, needles, and instruments. an additional duty of inspecting each instrument for loose or missing tape is stretching the limit. ID tape is just one more unnecessary worry for a harried nurse.
Microorganisms are crafty little devils and I suspect they could use the ID markings as a sort of shield to escape the unpleasant effects of gas or heat sterilization. I always suspected that tape margin where it interfaces with the instrument surface as an area for assorted biomass crud build-up. Instruments just look cleaner without identification tape.
I usually tried to avoid pharmaceutical reps and medical equipment sales people like the plague. The very reserved German fellow that represented VMueller instruments was a source of information and a true expert on the care and feeding of surgical instruments. He summed up my feelings perfectly when he surveyed an instrument tray with ID tapes plastered on his beautiful product, "Dumkopfs!" he hollered followed by some German cuss words He did not have to explain who or what he was referring to while I nodded my head in somber agreement.
Monday, September 18, 2017
Nurse Motivators - Paying a Debt
Intraoperative X-rays meant the gowned and gloved were huddled face-to-face behind that protective lead curtain off in a distant corner. Personal space dissipated more rapidly than Bovie smoke as we sought to guard our gamete giving gonads from gamma rays. (Whew... I was able to stop myself this time before that darned alliteration got out of control.) I found myself squeezed into an eyeball to neck position with Alana, the young student nurse I was mentoring. I could not curtail my stares to her neck and sub-mandible.
Now that was one impressive mass of scar tissue stretching from her clavicle and encircling her neck before terminating just below her jaw. A matrix of jagged spider web like connective tissue stacked as if one web was piled on top of another. I started to ponder what her skin graft donor sites looked like. Despite her sunny demeanor she had been through some significant suffering. Every minor turn of her head against that scar tissue looked like an activity resembling a taffy pull. No wonder she rotated her entire upper torso when scanning the operative field.
As I briefly pondered the backstory here, our eyes made contact and I quickly diverted my gaze, wondering if I should apologize for my crude fixed gaze. Maybe I could come up with a foolish excuse blaming it on the X-ray and being forced to position myself eyeball to neck. I never was known as a v ery subtle person and it was probably time for some soul searching. Maybe I could make it up to her by teaching her how to load a sponge stick one-handed. She was one of the most gung ho students I worked with.
ery subtle person and it was probably time for some soul searching. Maybe I could make it up to her by teaching her how to load a sponge stick one-handed. She was one of the most gung ho students I worked with.
After the case in the OR lounge I was bumbling and stumbling through a summary of the case while complimenting Alana on doing so well. When I started my uncomfortable mumbling regarding the indication for the intraoperative X-ray she sensed my uneasiness and simply replied, " The burn injury happened on a camping trip near the Wisconsin Dells when I was 8 years old. The fuel tank on the cookstove leaked and sprayed me with burning fuel. The nurses on the burn unit at County saved my life and I always felt in debt to them for their skill and many kindnesses. I decided to be a nurse on the day I walked out of that hospital."
Student nurses had diverse motivations for studying nursing, but decades ago it's a fact that money was not one of them. Alana's motivation was pure and simple, she was repaying a debt and it had nothing to do with remuneration.
How it became a debt for Alana is not too hard to understand. She felt the nurses on the burn unit at County gave her life back and she owed that much to others. In a fictional account, Alana would return to the County Burn Unit upon graduation and care for patients she could directly identify with.
The truth of the matter - Alana really like OR nursing and made that a career choice. Whenever I was weary or cynical with negativity barking at my heals, Alana's pure and simple motivation set me straight. As long as I was still vertical on the outside of the siderails, I owed a debt too. It brought tears to my foolish eyes when Alana related she decided to become an OR nurse after her very first scrub-in which happened to be with me.
As time passed, I tried to watch Alana in action every chance I had. Her hands were half the size of mine, but the way she spun a curved instrument in midair to pass it to either side of the table or police her Mayo stand was a mirror image of my technique. We even cut ligatures and wringed out lap sponges the exact same way. I simply loved watching her scrubbed and I never stared at her scar again.
.
Now that was one impressive mass of scar tissue stretching from her clavicle and encircling her neck before terminating just below her jaw. A matrix of jagged spider web like connective tissue stacked as if one web was piled on top of another. I started to ponder what her skin graft donor sites looked like. Despite her sunny demeanor she had been through some significant suffering. Every minor turn of her head against that scar tissue looked like an activity resembling a taffy pull. No wonder she rotated her entire upper torso when scanning the operative field.
As I briefly pondered the backstory here, our eyes made contact and I quickly diverted my gaze, wondering if I should apologize for my crude fixed gaze. Maybe I could come up with a foolish excuse blaming it on the X-ray and being forced to position myself eyeball to neck. I never was known as a v
 ery subtle person and it was probably time for some soul searching. Maybe I could make it up to her by teaching her how to load a sponge stick one-handed. She was one of the most gung ho students I worked with.
ery subtle person and it was probably time for some soul searching. Maybe I could make it up to her by teaching her how to load a sponge stick one-handed. She was one of the most gung ho students I worked with.After the case in the OR lounge I was bumbling and stumbling through a summary of the case while complimenting Alana on doing so well. When I started my uncomfortable mumbling regarding the indication for the intraoperative X-ray she sensed my uneasiness and simply replied, " The burn injury happened on a camping trip near the Wisconsin Dells when I was 8 years old. The fuel tank on the cookstove leaked and sprayed me with burning fuel. The nurses on the burn unit at County saved my life and I always felt in debt to them for their skill and many kindnesses. I decided to be a nurse on the day I walked out of that hospital."
Student nurses had diverse motivations for studying nursing, but decades ago it's a fact that money was not one of them. Alana's motivation was pure and simple, she was repaying a debt and it had nothing to do with remuneration.
How it became a debt for Alana is not too hard to understand. She felt the nurses on the burn unit at County gave her life back and she owed that much to others. In a fictional account, Alana would return to the County Burn Unit upon graduation and care for patients she could directly identify with.
The truth of the matter - Alana really like OR nursing and made that a career choice. Whenever I was weary or cynical with negativity barking at my heals, Alana's pure and simple motivation set me straight. As long as I was still vertical on the outside of the siderails, I owed a debt too. It brought tears to my foolish eyes when Alana related she decided to become an OR nurse after her very first scrub-in which happened to be with me.
As time passed, I tried to watch Alana in action every chance I had. Her hands were half the size of mine, but the way she spun a curved instrument in midair to pass it to either side of the table or police her Mayo stand was a mirror image of my technique. We even cut ligatures and wringed out lap sponges the exact same way. I simply loved watching her scrubbed and I never stared at her scar again.
.
Tuesday, September 12, 2017
Tonsillectomy According to Peter Ponsil
It's probably one of the pioneers in patient education, but the rosy picture it painted of tonsillectomy was bending the truth more than a triffle. Pediatric patients were told many half truths and outright fibs to gain their cooperation. Every old peds nurse knows that sneaky trick of telling little Peter Ponsil that it's time to check his temperature and then administering a painful intramuscular injection. That old Vistaril pre-op shot used to burn like a branding iron Misleading youngsters to gain their cooperation was just plain wrong, but I never had much of a say with older nurses.
Peter Ponsil conveniently neglected to mention some of the complications and post op
The most unusual complication I witnessed involved removing the uvula along with a tonsil. The surgeon told the family not to worry because the little thing hanging down in the back of the throat was unnecessary and just got in the way. He was half right - it did indeed get in the way of his snare.
Another youngster had to make an emergent trip back to the OR for a bronchoscopy because the eschar sloughed off a tonsillectomy wound and lodged in his right main stem bronchus. I think our friend Peter Ponsil would be singing a different tune post-bronchoscopy.
Our pediatric unit was divided into 3 separate wards: pre-op, post-op, and isolation which was affectionately known as the diarrhea ward. The unsuspecting kids in pre-op frolicked about in their Johnny Coats consumed by blissful ignorance courtesy of Peter Ponsil and his ilk. Post-op was where the reality of the situation reared it's ugly head. Kids howling in pain suddenly aware of how deceitful their friend, Pete, had been. The more rambunctious were even restrained on papoose boards. Peter Ponsil was a spin doctor of the highest order.
There was a great deal of deception in old school healthcare and Peter Ponsil bunches it all up in his little song that represents an entourage of hospital falsehoods. From nurses telling patients that a Bicillin injection would feel like a mosquito bite to surgeons obscuring an ominous finding, half truths and outright deception was everywhere. The pain word was beclouded by referring to it as discomfort. Of course this was all done for the patient's own good.
Thursday, September 7, 2017
Surgery Themed Establishments
DATELINE: Cairo, Egypt....Practicing surgeons have opened a surgery themed restaurant named D.Kebbda in mid-July where they are festooned in surgical scrubs and prepare their sole offering, grilled beef liver sandwiches behind an enclosed glass kitchen. Kebda is a popular street food in Egypt, but a vector of food poisoning if not prepared with caution. "We tried to take our career values and apply them to another field," said Mostafa Baisourny one of the owners. "There is no contradiction here, we are still practicing doctors."
This news item got me to thinking about other possibilities for other surgery themed businesses such as a surgical amusement park. One of the attractions would be to take a spin, so to speak, on the orthopedic traction table. Adduct an arm, abduct a leg and add some acute hip flexion and pretty soon you are twisted up like a pretzel. If you want to spend some time in that unique position just ask the friendly ride attendant to apply the plaster. What fun!
A carnivalesque side show might include an amazing sword swallowing act complete with an old school rigid metal bronchoscope. Those things were brutal and don't forget to duck the flying bits of mucous.
How about a combination buffet and Bariatric surgical center. Everyone enjoys one last big fling before their problem is addressed. Welcome to Stuff N' Cut where after enjoying a 9,000 calory last meal, bypass surgery is performed. Don't fret we wait out the prescribed time interval to avert aspiration.
I better cease this foolishness before it gets out of hand. Thanks so much for indulging in my outright preposterousness and a special shout out to you high minded academic types. My readership surges when school is in session.
This news item got me to thinking about other possibilities for other surgery themed businesses such as a surgical amusement park. One of the attractions would be to take a spin, so to speak, on the orthopedic traction table. Adduct an arm, abduct a leg and add some acute hip flexion and pretty soon you are twisted up like a pretzel. If you want to spend some time in that unique position just ask the friendly ride attendant to apply the plaster. What fun!
A carnivalesque side show might include an amazing sword swallowing act complete with an old school rigid metal bronchoscope. Those things were brutal and don't forget to duck the flying bits of mucous.
How about a combination buffet and Bariatric surgical center. Everyone enjoys one last big fling before their problem is addressed. Welcome to Stuff N' Cut where after enjoying a 9,000 calory last meal, bypass surgery is performed. Don't fret we wait out the prescribed time interval to avert aspiration.
I better cease this foolishness before it gets out of hand. Thanks so much for indulging in my outright preposterousness and a special shout out to you high minded academic types. My readership surges when school is in session.
Saturday, September 2, 2017
PAIN (Purposeful Affliction Isn't Nice)
Nursing presents the practitioner with an assortment of mind boggling difficult and unpleasant (to say the least) circumstances. Putrid and pungent odors, horrific sights of blood and gore along with unimaginable suffering. Every nurse has an Achille's Heal of a hospital situation that brings forth light headedness, tears and a cold sweat. For some it was blood and or trauma, Bovie smoke got to others, and odors elicited a vaso vagal response in many.
My weak spot was seeing patients in pain, all pain was blood curdling to my soul, but the inadvertently inflicted avoidable pain was what really what got caught in my craw. Needless suffering was the stuff of real nightmares for me. So in a lame attempt to unburden my tortured soul here is a laundry list of completely avoidable painful events I witnessed over the years. When I have trouble coming up with a coherent post on a single subject, laundry lists are my best friend.
This one really rankles my hackles and I always tried to put a halt to it when I was a circulating nurse in the OR. Eager beaver, out to impress, surgical residents sometimes jump the gun with inserting Foleys or starting lines before the patient is anesthetized. "Whoa not so fast, Dr. Speedy, how would you like that done while you are awake?" usually put a halt to the proceedings. Keeping Foley trays and other pre anesthesia induction paraphernalia out of sight until the patient was asleep was another effective tactic.
Last minute pre-op exams involving probing wounds or orifices could be stoped dead in their tracks by a good hard smack to the back of the hand with a sponge ring forceps. I never had the temerity to do this, but Alice my beloved supervisor was an equal opportunity sponge stick smacker. Anyone committing a wrongful act was fair game for aching knuckles. A crude but very effective deterrent that I have personally experienced. OUCH!
Hair follicles share the same neighborhood as sensory nerve endings so extricating hair really does smart, a fact some girls know all too well. My usual place to hang out in nursing school was in the lobby right next to the elevator. Occasionally nursing school stressors promoted disagreements among students which then led to hair-pulling donnybrooks. Standard procedure involved forcing the combatants into the elevator and hitting the down button for student nurse Fool to break up by squeezing the hand of the aggressor. I never knew what to expect when that elevator door opened but screams emanating from the elevator shaft was never a good sign. Somehow I was able to peacefully resolve the altercations, but the clumps of hair on the elevator floor always turned my stomach.
Every nurse is well versed in the inexcusable pain inflicted by aggressive adhesive tape removal. Kind hearted nurses knew that moistening the adhesive/skin interface zone with acetone helped minimize the hair pulling. Whether to remove adhesive tape slowly or rapidly was a hotly debated topic in nursing school. I always thought that giving the patient a choice was best and if they expressed a desire self removal, let them have a go at it. At least I was not the culprit inflicting pain.
Here is an unusual and little known unjustifiable hair pulling event that can occur in a very sensitive anatomical site. Pelvic exams place the patient in a vulnerable position and novice physicians have been known to entangle and twist pubic hairs out with those old metal speculums adjusted with set screws. The hair gets caught in the inclined plane of the set screw and subsequent adjustment yanks pubic hair out lickety-split. One of the reasons nurses were taught to always carry scissors was to cut free entangled hair.
Of all the surgical instruments, it's not those ghastly saws or chisels on top 10 lists that elicit revulsion in any sentient being - my vote goes to misused towel clips.. These innocent looking devices have two very sharp points that can be engaged by opening and closing the clip like a scissors. They were designed to securely attach towels to each other while draping. The practice of surgeons affixing towels directly to patients skin was history, but anesthetists found a use for towel clips that was unsavory at best.
The tips of the towel clip were engaged in the patient's skin at various levels to gauge the level of spinal anesthesia. When the patient screamed it was obviously the limit of the spinal's effectiveness. There were few of these towel clip wielding anesthetists, but just one is far too many.
Although never witnessed, I have heard horror stories of old time OB practitioners engaging the points of towel clips in a patient's hip to test their saddle block causing new mothers to wonder what demented doctor depredated derieres - developing devious deep puncture wounds (please excuse the alliteration, it's one of my very bad habits.)
Surgeons from my generation simply loved silk sutures and some even proudly bragged about being a "silk man." Surgical knots never slipped on silk sutures and they never assumed a coiled or unwieldy shape. The nature of these suture's surface was akin to a lattice-like structure owing to the fact they were braided from many fine silk strands. As tissue healed, it became enmeshed in these tiny lattice spaces. Removing silk skin sutures was like trying to pull a bone from a dog's mouth - lots of resistance and growling.
Surgical staple clips put an end to the misery of silk suture removal but many older surgeons wanted to remain loyal to the history of surgery and refused to accept them. Previous surgeries could be easily identified by the archaeologic artifacts left behind by black silk sutures. They were highly visible and always a sure sign that man had been in this wound before.
I'm getting off track so it must be time to wrap this post up but minimizing discomfort or aiding a patient in pain is something a nurse can do to minimize hopelessness and promote healing and recovery. A trauma patient will never notice how carefully a scrub nurse cuts ligatures but will always remember if they were patient and caring when transferring them from a Gurney to the table.
My weak spot was seeing patients in pain, all pain was blood curdling to my soul, but the inadvertently inflicted avoidable pain was what really what got caught in my craw. Needless suffering was the stuff of real nightmares for me. So in a lame attempt to unburden my tortured soul here is a laundry list of completely avoidable painful events I witnessed over the years. When I have trouble coming up with a coherent post on a single subject, laundry lists are my best friend.
This one really rankles my hackles and I always tried to put a halt to it when I was a circulating nurse in the OR. Eager beaver, out to impress, surgical residents sometimes jump the gun with inserting Foleys or starting lines before the patient is anesthetized. "Whoa not so fast, Dr. Speedy, how would you like that done while you are awake?" usually put a halt to the proceedings. Keeping Foley trays and other pre anesthesia induction paraphernalia out of sight until the patient was asleep was another effective tactic.
Last minute pre-op exams involving probing wounds or orifices could be stoped dead in their tracks by a good hard smack to the back of the hand with a sponge ring forceps. I never had the temerity to do this, but Alice my beloved supervisor was an equal opportunity sponge stick smacker. Anyone committing a wrongful act was fair game for aching knuckles. A crude but very effective deterrent that I have personally experienced. OUCH!
Hair follicles share the same neighborhood as sensory nerve endings so extricating hair really does smart, a fact some girls know all too well. My usual place to hang out in nursing school was in the lobby right next to the elevator. Occasionally nursing school stressors promoted disagreements among students which then led to hair-pulling donnybrooks. Standard procedure involved forcing the combatants into the elevator and hitting the down button for student nurse Fool to break up by squeezing the hand of the aggressor. I never knew what to expect when that elevator door opened but screams emanating from the elevator shaft was never a good sign. Somehow I was able to peacefully resolve the altercations, but the clumps of hair on the elevator floor always turned my stomach.
Every nurse is well versed in the inexcusable pain inflicted by aggressive adhesive tape removal. Kind hearted nurses knew that moistening the adhesive/skin interface zone with acetone helped minimize the hair pulling. Whether to remove adhesive tape slowly or rapidly was a hotly debated topic in nursing school. I always thought that giving the patient a choice was best and if they expressed a desire self removal, let them have a go at it. At least I was not the culprit inflicting pain.
Here is an unusual and little known unjustifiable hair pulling event that can occur in a very sensitive anatomical site. Pelvic exams place the patient in a vulnerable position and novice physicians have been known to entangle and twist pubic hairs out with those old metal speculums adjusted with set screws. The hair gets caught in the inclined plane of the set screw and subsequent adjustment yanks pubic hair out lickety-split. One of the reasons nurses were taught to always carry scissors was to cut free entangled hair.
Of all the surgical instruments, it's not those ghastly saws or chisels on top 10 lists that elicit revulsion in any sentient being - my vote goes to misused towel clips.. These innocent looking devices have two very sharp points that can be engaged by opening and closing the clip like a scissors. They were designed to securely attach towels to each other while draping. The practice of surgeons affixing towels directly to patients skin was history, but anesthetists found a use for towel clips that was unsavory at best.
 |
| Towel clips are for towels - not patients skin |
The tips of the towel clip were engaged in the patient's skin at various levels to gauge the level of spinal anesthesia. When the patient screamed it was obviously the limit of the spinal's effectiveness. There were few of these towel clip wielding anesthetists, but just one is far too many.
Although never witnessed, I have heard horror stories of old time OB practitioners engaging the points of towel clips in a patient's hip to test their saddle block causing new mothers to wonder what demented doctor depredated derieres - developing devious deep puncture wounds (please excuse the alliteration, it's one of my very bad habits.)
Surgeons from my generation simply loved silk sutures and some even proudly bragged about being a "silk man." Surgical knots never slipped on silk sutures and they never assumed a coiled or unwieldy shape. The nature of these suture's surface was akin to a lattice-like structure owing to the fact they were braided from many fine silk strands. As tissue healed, it became enmeshed in these tiny lattice spaces. Removing silk skin sutures was like trying to pull a bone from a dog's mouth - lots of resistance and growling.
Surgical staple clips put an end to the misery of silk suture removal but many older surgeons wanted to remain loyal to the history of surgery and refused to accept them. Previous surgeries could be easily identified by the archaeologic artifacts left behind by black silk sutures. They were highly visible and always a sure sign that man had been in this wound before.
I'm getting off track so it must be time to wrap this post up but minimizing discomfort or aiding a patient in pain is something a nurse can do to minimize hopelessness and promote healing and recovery. A trauma patient will never notice how carefully a scrub nurse cuts ligatures but will always remember if they were patient and caring when transferring them from a Gurney to the table.
Friday, August 25, 2017
Wednesday, August 23, 2017
Bridles Are for Horses - Not Patients
This post is about nursing interventions with nasogastric tubes from many decades ago and filtered through my aging nervous system so don't count on relevance. It's foolishness of the highest order for entertainment purposes only. With the advent of PEG tubes and a more enlightened attitude, hopefully bridlers are extinct.
Nasogastric tubes (NG tubes) were handy little devices. They were used post operatively and connected to low intermittent suction to decompress and keep the operative area clear after gastric surgery. Another use involved feeding patients that were unwilling or unable to take nourishment and this is where the problems showed up.
NG tubes were dangerous devices in the hands of an inexperienced practitioner and complications related to wrongful placement were sometimes devastating. The most common misplacement was in the lung via the right main stem bronchus (It's more perpendicular and bigger than the left bronchus) We always added a dash of methylene blue dye to feedings and if your patient coughed up blue mucous, it was a sign of trouble. The pleural regions are not known for their ability to assimilate nutrients and likewise there is little gas exchange across the stomach wall. It's best to respect these barriers and that's the understatement of all time!
 Skull fractures involving the cribiform plate invited the disaster of the NG tube winding up in the brain as shown on the right. Old time physicians hated to come clean with mistakes and I can just hear an old blow hard doc from the1960s coming up with a clever explanation that the NG tube in the X-ray could be used as a ventricular shunt, "after all it did course straight up the ventricle. Now we don't have to worry about complications like hydrocephalus."
Skull fractures involving the cribiform plate invited the disaster of the NG tube winding up in the brain as shown on the right. Old time physicians hated to come clean with mistakes and I can just hear an old blow hard doc from the1960s coming up with a clever explanation that the NG tube in the X-ray could be used as a ventricular shunt, "after all it did course straight up the ventricle. Now we don't have to worry about complications like hydrocephalus."
Blogger, Skeptical Scalpel has a fascinating post about an internal jugular vein cannulation by a misplaced NG tube. I think the person that accomplished this amazing feat blunder would have to fess up to the mistake. Who in the world ever heard of gaining vascular access via the nose? That phony excuse is just plain unbelievable.
Nurses commonly inserted NG feeding tubes and were responsible for keeping them in place. Post op patients were usually very cooperative as a result of vitamin "D" (Demerol) and did not tamper with their NG tubes. Placement of these NG tubes was also a short term affair of just a couple of days. It's much easier for a patient to put up with a short term nuisance than a long term festering aggravation.
Having an NG in place for a couple of weeks is a miserable experience that I have had personal experience with. Occluding a nostril for the tube results in forced mouth breathing that makes your throat dry as the Sahara dessert. Dried mucous referred to as snot in less formal arenas dries up around the tube and picking it off results in red sore nares.
Tubes like Foleys are out of the patient's view. NG tubes of yesteryear were a bright red in color and were like the matador's red cape to a bull - always annoying and always in sight. It's no surprise that patient's liked to remove their NG tubes. I always figured these poor old souls were trying to communicate something to us - they did not want tube feedings and their feelings should be respected. Leave the NG tube out and place a glass of water within reach.
Old nurses from the greatest generation had other ideas and I learned never to argue with these gallant geezers. All too often their interventions reflected their rigid, authoritarian personality and not the reality of the situation. They did not tolerate fools like me and their answer to patient self removal of NG tubes was a brutal but effective trick called NG tube bridling. Somehow these determined oldster nurses always prevailed when imposing their idea of therapeutic intervention.
Bridling involved inserting the NG tube via the right nostril until the tip of it was visible just below the uvuala (that funny thing hanging down between your tonsils.) I've been criticized for not writing clearly for non-medical folks, so that crude explanation is one of my lame attempts to be more broad based.
The old battle axe of a nurse then grabbed the NG tube from the back of the throat with a Magill forceps andgracefully pulled yanked the tube out the mouth. Some of these old Marquise de Sade nurses had tiny hands which meant they could skip the forceps and yank that bad boy NG tube out with their fingers. Once pulled all the way out via the mouth the NG tube was looped around and reinserted in the left nostril into the stomach.
The end result was the NG tube anatomically anchored because the loop went completely around the ethmoid bone and maxillary sinuses before it's descent back to the stomach. Pulling on the end of the NG tube resulted in excruciating pain which was an effective deterrent to removal. From my perspective, bridling was the stuff of nightmares with the poor patient yanking his nose and maxillary sinuses loose along with the offending NG tube.
I always tried to empathize with the patient. Dying patients just wanted peace and quiet on their lonely journey and before the hospice concept arrived this was rare. I always found a way out of the bridling NG tube business and only wish I could have had more influence on bridlers.
Nasogastric tubes (NG tubes) were handy little devices. They were used post operatively and connected to low intermittent suction to decompress and keep the operative area clear after gastric surgery. Another use involved feeding patients that were unwilling or unable to take nourishment and this is where the problems showed up.
NG tubes were dangerous devices in the hands of an inexperienced practitioner and complications related to wrongful placement were sometimes devastating. The most common misplacement was in the lung via the right main stem bronchus (It's more perpendicular and bigger than the left bronchus) We always added a dash of methylene blue dye to feedings and if your patient coughed up blue mucous, it was a sign of trouble. The pleural regions are not known for their ability to assimilate nutrients and likewise there is little gas exchange across the stomach wall. It's best to respect these barriers and that's the understatement of all time!
 Skull fractures involving the cribiform plate invited the disaster of the NG tube winding up in the brain as shown on the right. Old time physicians hated to come clean with mistakes and I can just hear an old blow hard doc from the1960s coming up with a clever explanation that the NG tube in the X-ray could be used as a ventricular shunt, "after all it did course straight up the ventricle. Now we don't have to worry about complications like hydrocephalus."
Skull fractures involving the cribiform plate invited the disaster of the NG tube winding up in the brain as shown on the right. Old time physicians hated to come clean with mistakes and I can just hear an old blow hard doc from the1960s coming up with a clever explanation that the NG tube in the X-ray could be used as a ventricular shunt, "after all it did course straight up the ventricle. Now we don't have to worry about complications like hydrocephalus."Blogger, Skeptical Scalpel has a fascinating post about an internal jugular vein cannulation by a misplaced NG tube. I think the person that accomplished this
Nurses commonly inserted NG feeding tubes and were responsible for keeping them in place. Post op patients were usually very cooperative as a result of vitamin "D" (Demerol) and did not tamper with their NG tubes. Placement of these NG tubes was also a short term affair of just a couple of days. It's much easier for a patient to put up with a short term nuisance than a long term festering aggravation.
Having an NG in place for a couple of weeks is a miserable experience that I have had personal experience with. Occluding a nostril for the tube results in forced mouth breathing that makes your throat dry as the Sahara dessert. Dried mucous referred to as snot in less formal arenas dries up around the tube and picking it off results in red sore nares.
Tubes like Foleys are out of the patient's view. NG tubes of yesteryear were a bright red in color and were like the matador's red cape to a bull - always annoying and always in sight. It's no surprise that patient's liked to remove their NG tubes. I always figured these poor old souls were trying to communicate something to us - they did not want tube feedings and their feelings should be respected. Leave the NG tube out and place a glass of water within reach.
Old nurses from the greatest generation had other ideas and I learned never to argue with these gallant geezers. All too often their interventions reflected their rigid, authoritarian personality and not the reality of the situation. They did not tolerate fools like me and their answer to patient self removal of NG tubes was a brutal but effective trick called NG tube bridling. Somehow these determined oldster nurses always prevailed when imposing their idea of therapeutic intervention.
Bridling involved inserting the NG tube via the right nostril until the tip of it was visible just below the uvuala (that funny thing hanging down between your tonsils.) I've been criticized for not writing clearly for non-medical folks, so that crude explanation is one of my lame attempts to be more broad based.
The old battle axe of a nurse then grabbed the NG tube from the back of the throat with a Magill forceps and
The end result was the NG tube anatomically anchored because the loop went completely around the ethmoid bone and maxillary sinuses before it's descent back to the stomach. Pulling on the end of the NG tube resulted in excruciating pain which was an effective deterrent to removal. From my perspective, bridling was the stuff of nightmares with the poor patient yanking his nose and maxillary sinuses loose along with the offending NG tube.
I always tried to empathize with the patient. Dying patients just wanted peace and quiet on their lonely journey and before the hospice concept arrived this was rare. I always found a way out of the bridling NG tube business and only wish I could have had more influence on bridlers.
Friday, August 18, 2017
Side Rail Peference Separates the Bedside Nurses from the Office Sitters
Any bedside nurse can attest to the fact that the only safe side rail on a hospital bed is one that runs the full length of the mattress from head to foot in a single section. All old school hand cranked beds had full siderails that were raised and lowered guillotine style or hinged to swing out and below the bed when giving care. My favorite was the straight up and down style release because the swinging rail bed had to be moved out from the wall to drop a rail. When dealing with a patient determined to exit stage right it is sometimes helpful to butt the bed against a wall as a containment aid.
Old full length side rails engaged with a reassuring clunk that meant business - similar to the feeling of a cycling shoe engaging with a clipless pedal - the patient is safe and I'm going to ride forever! At times it can be difficult to disengage from a bike pedal which always results in a fall for me, but I cannot recall any patient falls from an engaged full length side rail bed. Those old school side rails prized function over form which is the exact opposite of new fangled split side rails that are ubiquitous in today's hospital world..
Old full length side rails engaged with a reassuring clunk that meant business - similar to the feeling of a cycling shoe engaging with a clipless pedal - the patient is safe and I'm going to ride forever! At times it can be difficult to disengage from a bike pedal which always results in a fall for me, but I cannot recall any patient falls from an engaged full length side rail bed. Those old school side rails prized function over form which is the exact opposite of new fangled split side rails that are ubiquitous in today's hospital world..
The split rail special shown above is the office sitters dream bed and one big nightmare for the bedside practitioner. Sure it looks less intimidating and has better aesthetics than a full rail bed, but note the egress points between the foot of the bed and the bottom side rail. There is also an potential exit between the two rails that usually results in an extremity entrapment which is never pleasant. I've witnessed harried nurses lube up a patient's leg with Lubafax in a desperate attempt to slide it back to bed from under or between a siderail. Without the Lubafax those side rails are like Chinese handcuffs and the harder you yank on that leg, the more difficult it is to free.
Another fairly common exit strategy with this type of bed is often called the "flying buttress" for lack of a more technical name. The patient does a 45 degree rotation while prone and uses the bottom side rail to leverage his hips up and over the bed. It's prudent for a nurse to intervene while the buttress, so to speak, is still flying because the landing can be a real doozey when the patient impacts the floor. Thankfully most patients emit a verbal warning in the form of a shriek when they get stuck over the siderail and suspended in an uncomfortable, to say the least, position. At least the Surgilube or Lubafax is unnecessary with a flying buttress.
Today office sitting busy bodies are claiming that siderails are restraint devices which is pure balderdash to old nurses who like to think of them as freedom from falling incident devices. All an old nurse needs to keep just about any patient safe in bed is an extra sheet, a washcloth, and a roll of 3 inch gauze. The sheet is applied lengthwise across the patients chest and under the arms. The ends of the sheet are tied under the bed with the full length side rail up.
Mitts are applied by asking the patient to squeeze a rolled up wash cloth. The roll gauze is applied to the clenched fist from the wrist to fingertips creating a boxing gloved appearing hand. This also has the advantage of ceasing IV pulling or self adjustment of Foley catheters by the patient. I have seen motivated patients discontinue their NG tubes by clamping the tube between the mitts and yanking. This only happened once though because seasoned, old time nurses would bridle their NG tube by. OOPS never mind bridling - that's fodder for another post. Bridling of NG tubes is cruel and unusual punishment in my opinion and should never be done.
Egress minded patients are best kept far apart from each other. Semi private rooms become the devil's workshop if a couple of these bed bail out kings become buddies. Many times I have seen one patient perfect an exit strategy and then proceed to free his neighbor from bed. Once freed from the surly bonds of the hospital beds these folks just love to yank on Foleys, discontinue IVs and get into unimaginable mischief.
Full length side rails were highly functional and cost effective. Old hospital beds cost hundreds of dollars, not thousands like the beds of today. It's hard for me to fathom how something so highly functional could go by the wayside.
Today office sitting busy bodies are claiming that siderails are restraint devices which is pure balderdash to old nurses who like to think of them as freedom from falling incident devices. All an old nurse needs to keep just about any patient safe in bed is an extra sheet, a washcloth, and a roll of 3 inch gauze. The sheet is applied lengthwise across the patients chest and under the arms. The ends of the sheet are tied under the bed with the full length side rail up.
Mitts are applied by asking the patient to squeeze a rolled up wash cloth. The roll gauze is applied to the clenched fist from the wrist to fingertips creating a boxing gloved appearing hand. This also has the advantage of ceasing IV pulling or self adjustment of Foley catheters by the patient. I have seen motivated patients discontinue their NG tubes by clamping the tube between the mitts and yanking. This only happened once though because seasoned, old time nurses would bridle their NG tube by. OOPS never mind bridling - that's fodder for another post. Bridling of NG tubes is cruel and unusual punishment in my opinion and should never be done.
Egress minded patients are best kept far apart from each other. Semi private rooms become the devil's workshop if a couple of these bed bail out kings become buddies. Many times I have seen one patient perfect an exit strategy and then proceed to free his neighbor from bed. Once freed from the surly bonds of the hospital beds these folks just love to yank on Foleys, discontinue IVs and get into unimaginable mischief.
Full length side rails were highly functional and cost effective. Old hospital beds cost hundreds of dollars, not thousands like the beds of today. It's hard for me to fathom how something so highly functional could go by the wayside.
.
Subscribe to:
Posts (Atom)